January 9, 2023
12 Psychiatry Note Templates That Save Time
.webp)
Written by
Dr. Carlene MacMillan, MD
As a psychiatrist, you know firsthand how time-consuming and tedious documentation can be. It's easy to get bogged down in the paperwork, leaving little time for actually treating your patients.
But what if there was a way to streamline this process and save time on documentation? That's where psychiatry note templates come in. These pre-designed templates prompts provide a structured format for documenting various aspects of patient care, including evaluation, treatment, and follow-up—so you don’t have to reinvent the wheel.
Why should you use psychiatry note templates and smart phrases:
- Psychiatry note templates and smart phrases can save time and energy on documentation by providing a pre-formatted structure to follow.
- Templates can be especially helpful for routine tasks like follow-up visits or group therapy sessions.
- Using templates can help ensure that all necessary information is covered and regulatory requirements are met.
- Templates can also improve the quality of documentation by allowing for consistent tracking of changes in patients' conditions and identification of patterns or trends.
- Using templates and smart phrases can free up more time for providing patient care.
Templates let you quickly document your patient encounters, freeing up more time to focus on what really matters: providing the best possible care to your patients.
In this blog post, we'll delve into the various types of psychiatry note templates available and how they can save you time on documentation.
Follow-up SOAP Note Template for Psychiatrists
This template is used for documenting follow-up visits with patients. The SOAP (Subjective, Objective, Assessment, and Plan) format is commonly used in medical documentation and includes information about the patient's symptoms, a mental status examination, an assessment of the patient's condition, and a plan for further treatment or management. It should document the time spent face-to-face with the patient and any additional time spent that day on the patient’s care as well as documentation of the complexity of medical decision-making and any psychotherapy included in the visit. These elements are important for coding and billing accurately.
Family/Partner Therapy Note Template
This template is used for documenting therapy sessions with families, partners or couples. It should include information about who was present for the session, the goals of the therapy, the interventions used during the session, and any progress or changes in the treatment course.
Psychiatry History and Evaluation Note Template
This template is used for conducting an initial evaluation of a patient's mental health condition. It should include information about the patient's history, symptoms, any relevant physical or psychological examination findings, any data from rating scales or laboratory studies, and a thorough discussion of the differential diagnosis and plan. Ideally this note could easily import information completed by the patient during a prospective patient screening process.
Psychiatry Evaluation Note Template for Pediatric Patients
This template is similar to the Evaluation Note but is specifically designed for evaluating the mental health of pediatric patients. It should include additional information about the child’s developmental history, educational history, family/custody issues, hobbies, and summaries from any external reports such as school report cards or neuropsychological evaluations.
Group Therapy Note Template
This template is used for documenting group therapy sessions. It should include information about the number of attendees and any absent members, the format of the group, the overall focus of the group, and a few lines about the individual group member’s participation in the group. It should not contain any identifying information about other members of the group.
Order Note Template
This template is used for documenting orders for medications administered in the officer or other treatments or procedures a clinician is requesting. It should include information about the medication or treatment being ordered, the dosage and frequency, and any relevant instructions or precautions.
Telephone/SMS Encounter Note
This template is used for documenting encounters with patients over the phone or through text messaging. It should include information about the patient's symptoms, the interventions used during the encounter, the start and end time/total time spent and any progress or changes in the patient's condition.
Discharge From Practice Note Template
This template is used for documenting the process of discharging a patient from a practice. It should include information about the reason for the discharge, any follow-up recommendations, and any necessary referrals to other clinicians or services.
Crisis/Sentinel Event Note Template
This template is used for documenting a crisis or sentinel events, which are unexpected or significant events that have a negative impact on a patient's mental or physical health. It should include information about the event, the patient's response, and any interventions or follow-up recommendations.
Templates for Interventional Psychiatry Practices
Spravato (Esketamine) Note Template
This template is used for documenting treatment with the medication Spravato (esketamine), which is used for treatment-resistant depression. The template should include information about the REMS (Risk Evaluation and Mitigation Strategy) requirements for this medication, which are put in place by the FDA to ensure that the risks of using the medication are minimized.
TMS Treatment Note Template
This template is used for documenting treatment with transcranial magnetic stimulation (TMS), which is a non-invasive procedure that uses a magnet to stimulate specific areas of the brain. The template should include information on the treatment parameters used for the session, any changes to the patient’s clinical status that could impact the TMS treatment, information on the technician administering the treatment and an attestation by the supervising physician or nurse practitioner who will be signing off on the note.
IV/IM Ketamine Note Templates
These templates are used for documenting treatment with intravenous (IV) or intramuscular (IM) ketamine, which is a medication that is used off-label for treatment-resistant depression and other mental health conditions. The templates should include information about what was administered, timestamps, who administered the medication and any additional medications as well as vital signs throughout the treatment and any other notable aspects of the patient’s presentation on the day of the treatment.
Now you have an idea of which templates you'll use the most often. These just scratch the surface. Depending on your caseload, you may find yourself searching for a specific template, or modifying an existing one to fit your specific use case. Either way, you don’t need to reinvent the wheel—or wait until nights and weekends to finish your documentation.
Save time with Osmind's growing library of 60+ psychiatry templates
Within Osmind’s community, you’ll find clinicians sharing best practices for streamlining documentation time, cutting-edge research digests, and private practice growth strategies. You also get access to a growing library of over 60 templates. You can customize any template and create your own.
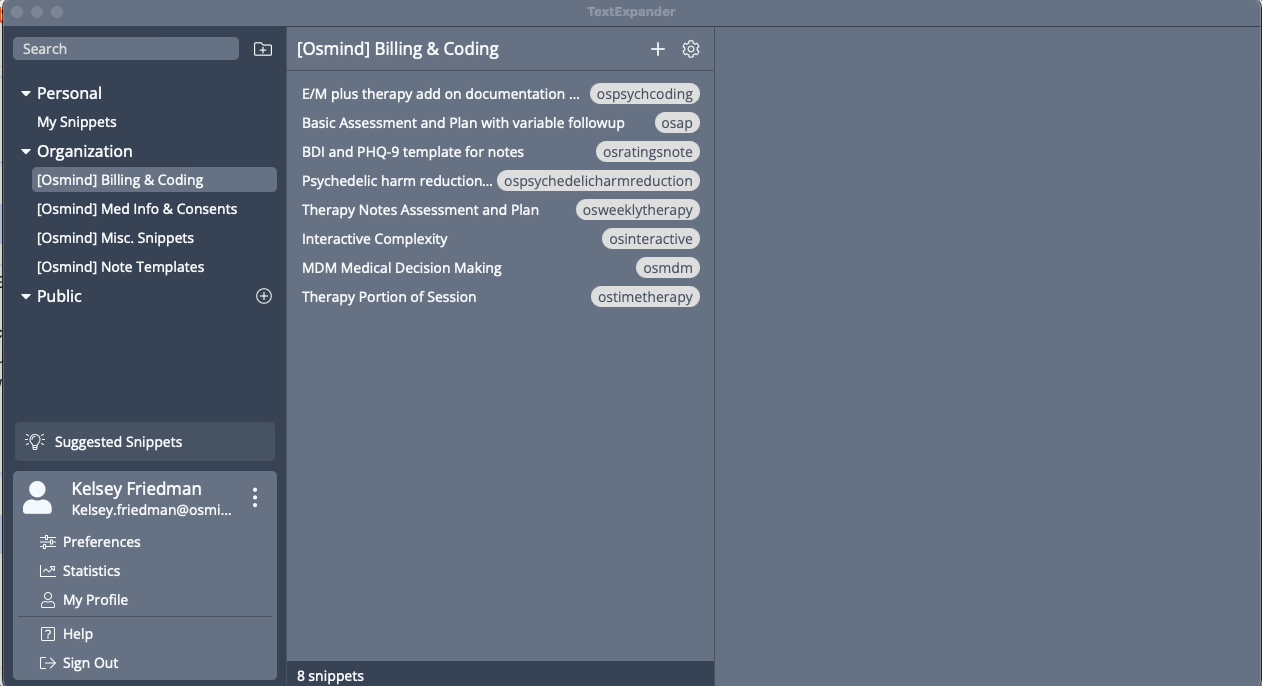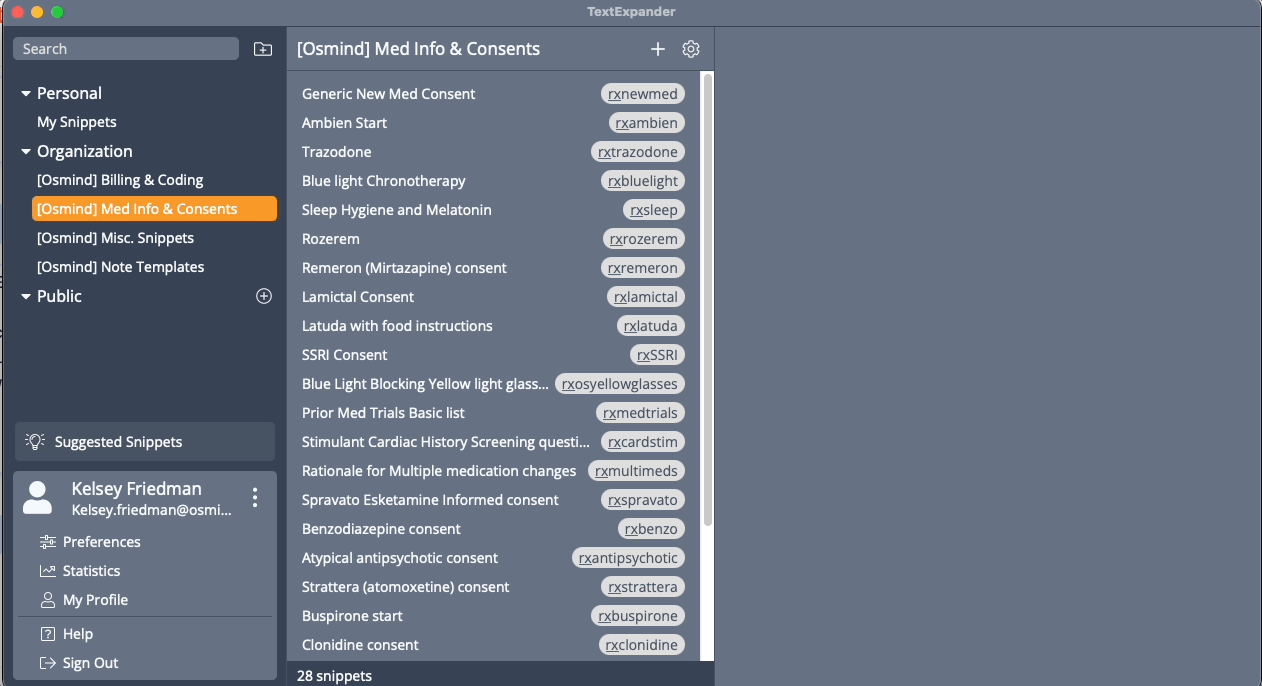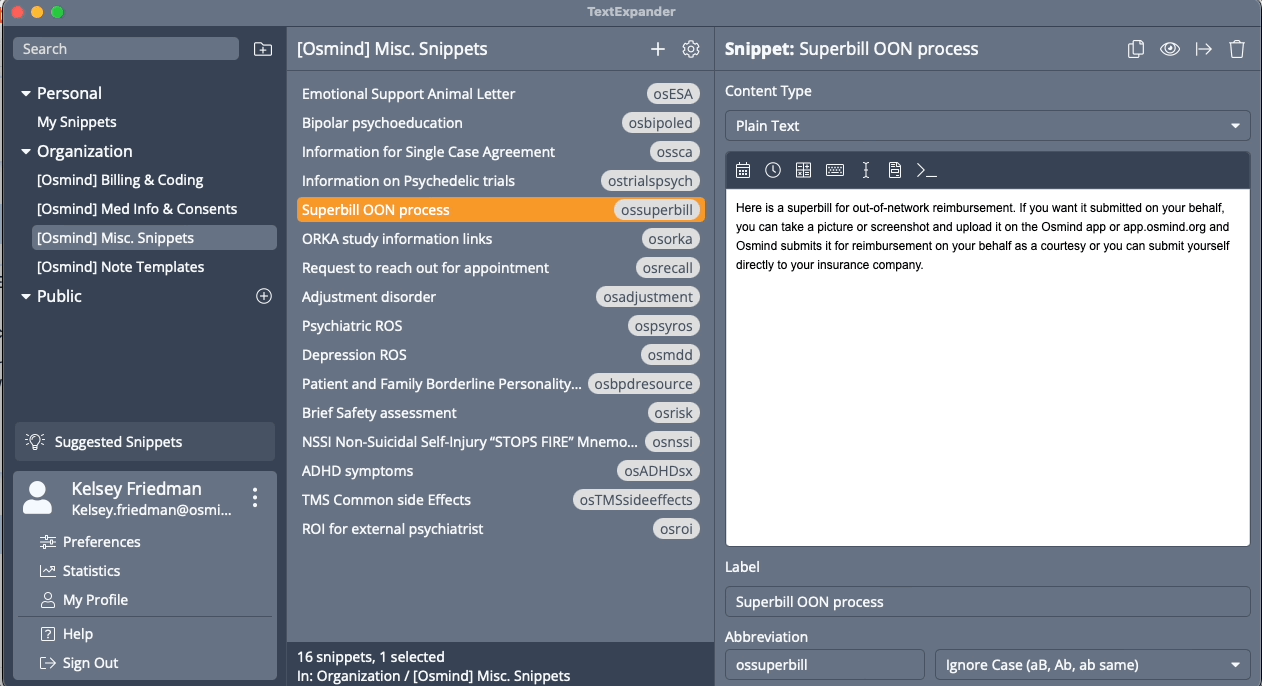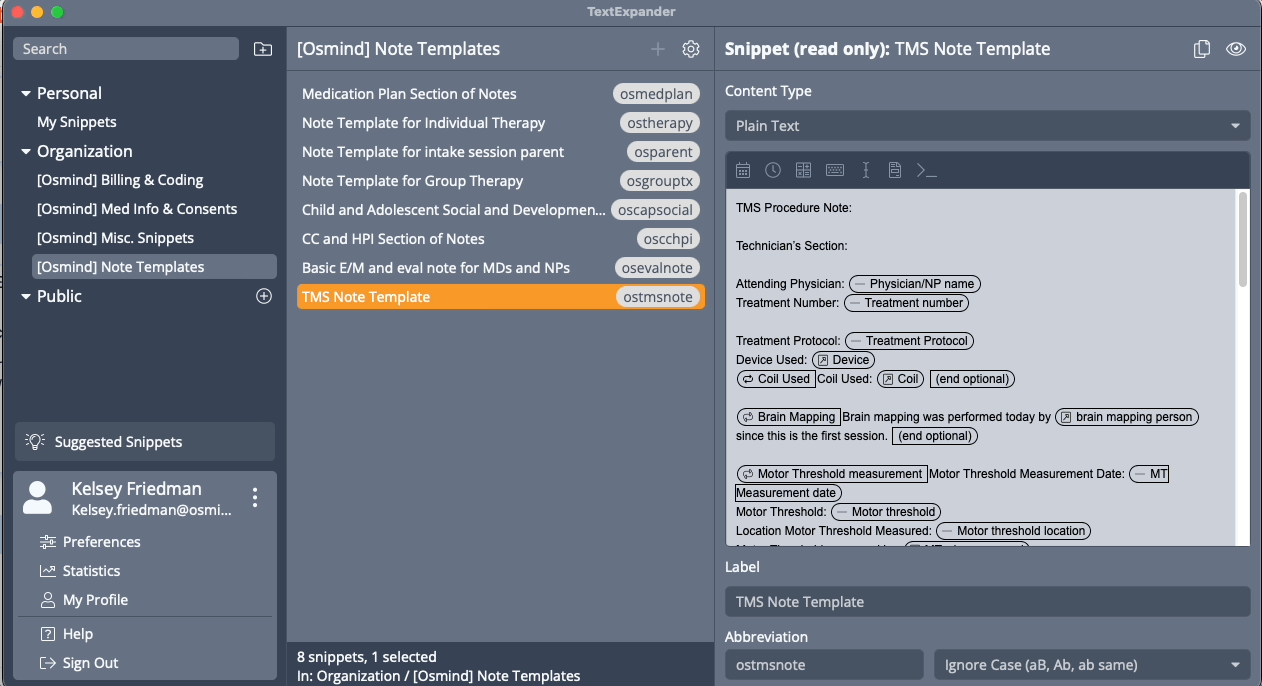
The best part? These templates and snippets can be used outside of Osmind—so you can save time anywhere you can type. You’ll have peace of mind knowing your documentation is consistent and accurate.
Conclusion:
Using psychiatry note templates can be a win-win for both you and your patients. By streamlining your documentation process, you can free up more time to focus on what really matters – providing the best possible care for your patients.
Ready to join the future of mental health? Learn how Osmind can streamline your practice and feel free to book a demo. We’re happy to answer all your questions and give tips for saving time on documentation and beyond.
Connect with forward-thinking peers, advance your practice, and attend expert events. Join the Psychiatry Collective today.
If you, or someone you know, is in crisis or needs immediate assistance, please call 911 immediately. To talk to someone now, please call the National Suicide Prevention Lifeline at 1-800-273-8255 or 988.
Osmind © 2026 All Rights Reserved.




.png)
.png)
.png)

.webp)
